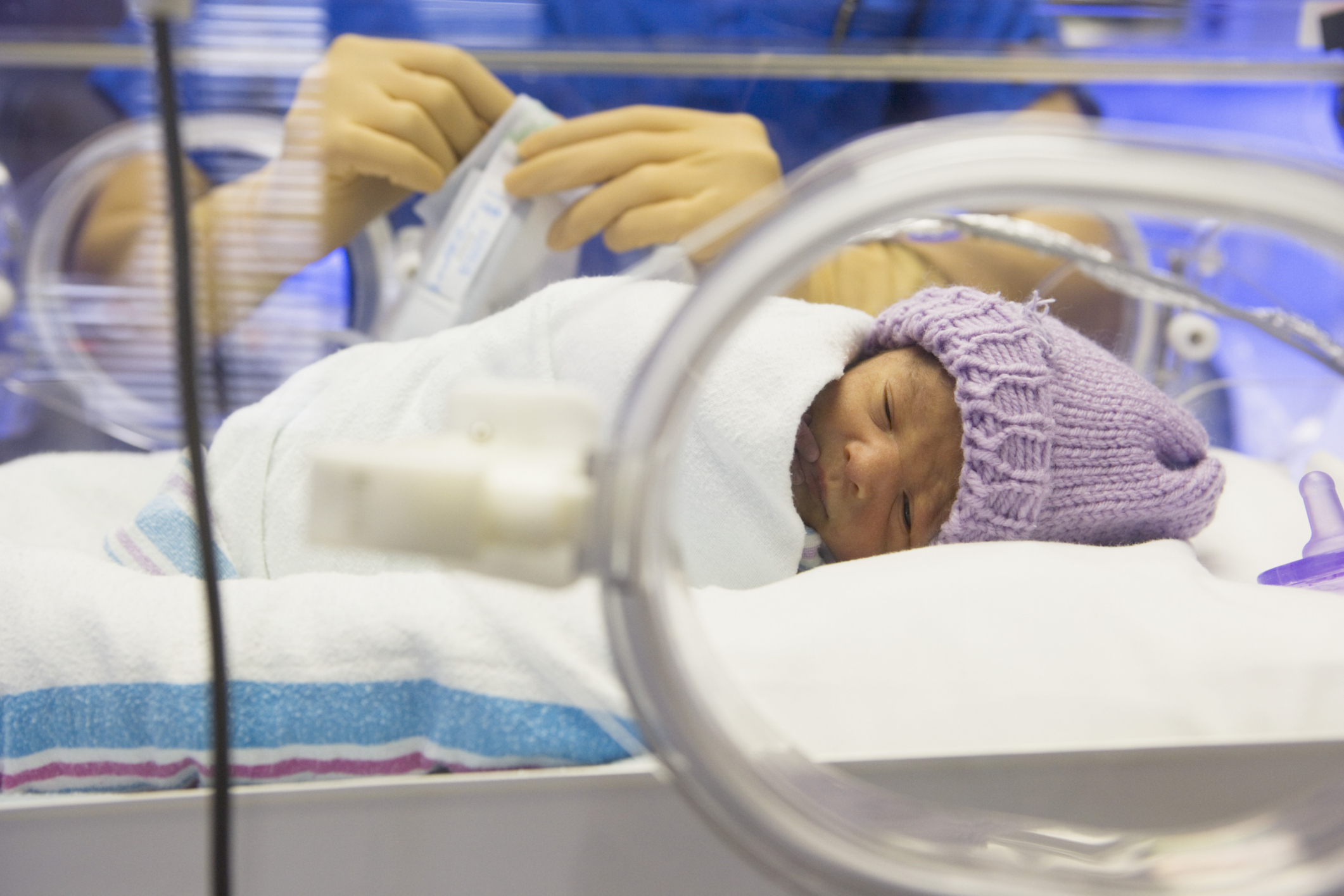
If you or your baby are unwell, you may wonder whether it’s safe to breastfeed. The good news is breastfeeding while sick can have many benefits for both of you – read on to find out more.
Did you know that if you breastfeed, your baby is less likely to get ill in the first place? While it won’t completely stop her becoming sick, breast milk’s protective properties mean breastfed babies tend to be unwell less often,1 and recover faster, than formula-fed babies.
Breast milk has antibacterial and antiviral elements.2 Depending on how long you breastfeed for, you’ll be lowering your baby’s risk of contracting colds and flu, ear and respiratory tract infections, sickness and diarrhoea.1 Scientists are even investigating breast milk’s potential for treating conditions ranging from conjunctivitis to cancer.3,4
Should I breastfeed my sick infant?
Yes. Breastfeeding a sick baby gives her a great chance of a speedy recovery, as well as helping to comfort her. Your breast milk contains antibodies, white blood cells, stem cells and protective enzymes that fight infections and may help with healing.1,5,6 It also has a constantly adjusting balance of vitamins and nutrients, supporting her to get better as quickly as possible. And that means fewer sick days and visits to the doctor for both of you.7
“Breastfeeding provides everything your baby needs if she’s poorly – it’s her medicine as well as her food, fluid and comfort. It’s the best thing on the planet for her,” says Sarah Beeson, a UK-based health visitor and nurse.
Amazingly, the composition of your breast milk changes when your baby is ill. If you’re exposed to a bacterial or viral infection, your body makes antibodies to combat it; these are then transferred to your baby through your milk.8 The levels of immunity-boosting cells, called leukocytes, in your milk also rise rapidly whenever your baby is unwell.5
And because breast milk is very easy to digest, it’s also the ideal food for babies with upset tummies.
“My daughter contracted norovirus when she was 12 months old, and breast milk was the only thing she could keep down,” remembers Maya, mum of two, Spain. We had weaned naturally to one breastfeed a day at bedtime, but the supply-and-demand effect of breastfeeding her more often again was quite astonishing. Within 48 hours, I was at dairy levels of production! It saved my baby girl being put on a drip.”
Bear in mind that you may have to alter the way you breastfeed your baby while she is sick. For example, a baby with a cold may want to feed more often, but for shorter periods, both for comfort and because a blocked nose may make it harder to stay at the breast for long. If your baby has a stuffy nose she might also prefer to feed upright, so you could experiment with different breastfeeding positions.
What if my baby seems too unwell to breastfeed?
Sometimes when a baby is feeling really ill she may not have the appetite or energy to breastfeed. If you’re struggling to get her to feed, contact a healthcare professional, lactation consultant or breastfeeding specialist for advice to prevent her becoming dehydrated.
They may advise you to express some milk to feed to your baby from a syringe, cup, or other method that you’ve found requires the least effort from her to drink from. Expressing when you would normally breastfeed will also keep your milk supply steady.
If you have any concerns about your baby’s health or milk intake, always seek medical advice quickly.
Can I still breastfeed when sick?
It may be the last thing you feel like doing, but it’s best to keep breastfeeding through almost any common illness. If you have a cold or flu, fever, diarrhoea and vomiting, or mastitis, keep breastfeeding as normal. Your baby won’t catch the illness through your breast milk – in fact, it will contain antibodies to reduce her risk of getting the same bug.
“Not only is it safe, breastfeeding while sick is a good idea. Your baby is actually the person least likely to fall ill with your tummy upset or cold, as she has already been in close contact with you and is getting a daily dose of those protective antibodies from your milk,” says Sarah Beeson.
However, being sick and continuing to breastfeed can be extremely tiring. You’ll need to look after yourself so you can look after your baby. Keep your fluid levels up, eat when you can, and remember your body needs extra rest. Book a seat on your sofa and snuggle up with your baby for a few days, and ask family or friends to help with caring for your baby when possible so you can focus on recovering.
“Don’t worry about your breast milk supply – you will keep producing it. Just don’t stop breastfeeding abruptly as you’ll run the risk of getting mastitis,” Sarah adds.
Good hygiene is important to minimise the risk of spreading the illness. Wash your hands with soap before and after feeding your baby, preparing and eating food, going to the toilet or changing nappies. Catch coughs and sneezes in a tissue, or in the crook of your elbow (not your hands) if you don’t have one with you, and always wash or sanitise your hands after coughing, sneezing or blowing your nose.
Is it OK to take medicines while breastfeeding?
It’s fine to take paracetamol, ibuprofen and some antibiotics while breastfeeding,9,10 as long as you discuss it with a healthcare professional and follow the dosing instructions. Remember ibuprofen has contraindications for asthmatic mums.
Previously mums were advised to avoid aspirin, but a recent study indicated low doses are likely to be safe while breastfeeding.11 However, high doses have been linked to a rare but serious condition called Reye’s syndrome in infants,12 so it’s best to discuss the use of aspirin with your healthcare professional.
Stronger prescription painkillers, such as codeine and tramadol, aren’t recommended.10 Since guidelines and recommendations are continually updated, your healthcare professional or pharmacist will be able to give you more information on specific medicines if you have any concerns.
Some cold, flu and cough remedies contain decongestants or expectorants, and these could reduce your milk supply. Steer clear of those that have phenylephrine, phenylpropanolamine or guaifenesin listed in their ingredients.9 Medicines that cause drowsiness are best avoided when you’re breastfeeding too.
“Check the packaging and if you’re still uncertain, ask a healthcare professional,” Sarah advises. “And if your baby was born prematurely, at a low birth weight, or has a medical condition, you should check before taking any medications while breastfeeding – even paracetamol.”
“Whenever you go to a doctor or a pharmacist, for any reason, always make it clear you’re breastfeeding and ask for the best option,” she adds.
How about long-term medication?
If you’re on long-term medication for diabetes, asthma, depression or any other chronic health condition, the benefits of breastfeeding can outweigh the risks. “Breastfeeding is often still possible with nearly all illnesses, except for a few rare conditions,” says Sarah. “You’ll be familiar with your regular medications and should have an opportunity to discuss them with your doctor or specialist while pregnant. There is guidance available for all healthcare professionals on the safety of different drugs.” In any event, you should discuss this issue with your doctor or healthcare professional.
I was on a high dose of medication for my epilepsy but breastfeeding was still possible,” says Nicola, mum of one, UK. “I was monitored by my neurologist to get a balance between safety for my son and keeping my risk of a seizure low. Seizures can be triggered by lack of sleep and I was feeding day and night, but I took good care of myself, as did my husband. It’s been a positive experience.”
What if I have to go into hospital?
Whether you need planned or emergency treatment, there are ways to ensure your baby continues to receive the benefits of breast milk, and that you can continue breastfeeding once discharged.
“Express and freeze your breast milk so a caregiver can feed it to your baby. Have a practice ahead of time, and make sure you tell healthcare professionals you are a breastfeeding mum when you’re booked in, and again when you’re admitted,” suggests Sarah.
“If your baby is small, they may let you have her with you. Ask whether there’s a hospital lactation consultant or breastfeeding specialist you can see too – they’ll be a great advocate for you, especially if you’re on a general ward. If it’s an emergency, make sure the healthcare professionals know you have a baby – it’s not something they might think about otherwise.”
Having surgery under local or general anaesthetic doesn’t mean you need to stop breastfeeding, or to ‘pump and dump’ your breast milk. By the time you feel well enough to hold your baby after an operation, the amount of anaesthetic in your breast milk will be minimal and it should nearly always be safe to breastfeed.10 However, you should seek the advice of a healthcare professional, lactation consultant or breastfeeding specialist in any of these circumstances.
Should I ever not breastfeed?
There are a few situations in which it’s safest to stop breastfeeding temporarily and pump and discard your milk to keep up your supply until treatment is complete. These include if you have radiotherapy or chemotherapy for cancer, herpes lesions on your breast, or infections such as tuberculosis, measles or septicaemia, that could be transmitted through your milk.13,14 Seek expert medical advice about your condition and whether it’s best to continue or interrupt breastfeeding.
- Victora CG et al. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet. 2016;387(10017):475-490.
- Lönnerdal B. Bioactive proteins in breast milk. J Paediatr Child Health. 2013;49 Suppl 1:1-7.
- Australian Breastfeeding Association [Internet]. Topical treatment with breastmilk: randomised trials. [cited 2018 Apr 4]. Available from https://www.breastfeeding.asn.au/tropical-treatment-with-breastmilk-randomised-trials
- Ho JCS et al. HAMLET–A protein-lipid complex with broad tumoricidal activity. Biochem Biophys Res Commun. 2017;482(3):454-458.
- Hassiotou F et al. Maternal and infant infections stimulate a rapid leukocyte response in breastmilk. Clin Transl Immunology. 2013;2(4):e3.
- Hassiotou F, Hartmann PE. At the dawn of a new discovery: the potential of breast milk stem cells. Adv Nutr. 2014;5(6):770-778.
- Ladomenou F et al. Protective effect of exclusive breastfeeding against infections during infancy: a prospective study. Arch Dis Child. 2010;95(12):1004-1008.
- Hanson LA. Breastfeeding provides passive and likely long-lasting active immunity. Ann Allergy Asthma Immunol. 1998;81(6):523-533.
- Hale TW, Rowe HE. Medications and Mothers’ Milk 2017. 17th ed. New York, USA: Springer Publishing Company; 2017. 1095 p.
- Reece-Stremtan S et al. ABM Clinical Protocol# 15: Analgesia and anesthesia for the breastfeeding mother, Revised 2017. Breastfeed Med. 2017;12(9):500-506.
- Datta P et al. Transfer of low dose aspirin into human milk. J Hum Lact. 2017;33(2):296-299.
- Morello O. Safe in breastfeeding [Internet]. Italy: Orfeo Morello; 2016. Aspirin: Can I take aspirin while breastfeeding? [cited 2018 Apr 4]. Available from: https://www.safeinbreastfeeding.com/aspirin/
- Lamounier JA et al. Recommendations for breastfeeding during maternal infections. J Pediatr (Rio J). 2004;80(5 Suppl):181-188.
- Hema M et al., Management of newborn infant born to mother suffering from tuberculosis: Current recommendations & gaps in knowledge. Indian J Med Res. 2014;140(1):32-39.